|
Getting your Trinity Audio player ready...
|
Orthostatic hypotension, also referred to as postural hypotension, is a medical condition characterized by a sudden drop in blood pressure when a person stands up from a sitting or lying position. This article will delve into the causes, symptoms, risk factors, complications, diagnosis, and treatment of orthostatic hypotension.
Table of Contents
What is Orthostatic Hypotension?
Orthostatic hypotension is a form of low blood pressure that occurs upon standing from a sitting or lying down position. This condition can cause feelings of lightheadedness, dizziness, and even fainting. Orthostatic hypotension is often common among the elderly and other individuals with low blood pressure.
Signs and Symptoms of Orthostatic Hypotension
The most common symptom of orthostatic hypotension is lightheadedness or dizziness when standing up after sitting or lying down. These symptoms typically last less than a few minutes. However, some individuals may experience more severe symptoms, such as:
- Blurry vision
- Weakness
- Fainting (also known as syncope)
- Confusion
In some cases, orthostatic hypotension may cause no symptoms. However, it’s important to consult a healthcare provider if you frequently feel lightheaded when standing up, as this could indicate a more serious underlying health problem.
When to See a Doctor
While occasional dizziness or lightheadedness can be insignificant — often triggered by mild dehydration, low blood sugar, or overheating — it’s crucial to consult a healthcare provider if symptoms of orthostatic hypotension occur frequently. Losing consciousness, even for just a few seconds, is a serious matter that requires immediate medical attention.
Causes of Orthostatic Hypotension
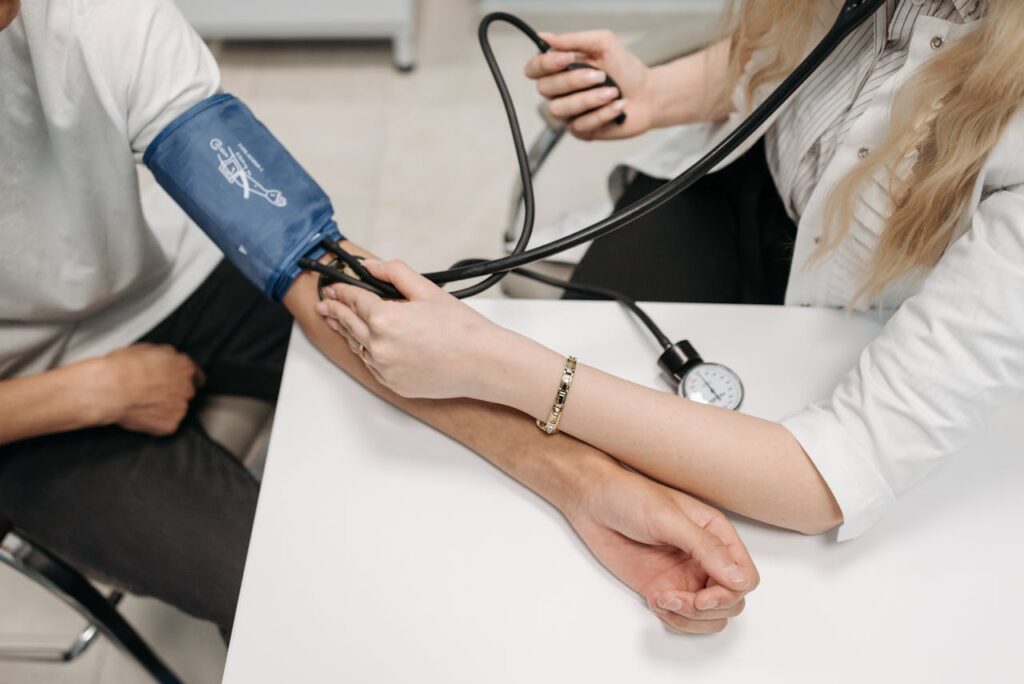
Orthostatic hypotension occurs when something interferes with the body’s natural process of counteracting low blood pressure. Many conditions can cause orthostatic hypotension, including:
- Dehydration: Conditions such as fever, vomiting, severe diarrhea, and strenuous exercise can lead to dehydration, which, in turn, can cause orthostatic hypotension.
- Heart problems: Conditions like extremely low heart rate (bradycardia), heart valve problems, heart attack, and heart failure can lead to low blood pressure.
- Endocrine problems: Conditions such as thyroid disorders, adrenal insufficiency (Addison’s disease), low blood sugar (hypoglycemia), and diabetes can cause orthostatic hypotension.
- Nervous system disorders: Disorders like Parkinson’s disease, multiple system atrophy, Lewy body dementia, pure autonomic failure, and amyloidosis can disrupt the body’s ability to control blood pressure.
Risk Factors Associated with Orthostatic Hypotension
Certain factors can increase the risk of orthostatic hypotension, including:
- Age: Orthostatic hypotension is common in individuals aged 65 and older.
- Medications: Medications used to treat high blood pressure, heart disease, Parkinson’s disease, depression, and erectile dysfunction can increase the risk of orthostatic hypotension.
- Certain diseases: Conditions such as heart disease, Parkinson’s disease, and diabetes can increase the risk of low blood pressure.
- Heat exposure: Being in a hot environment can cause heavy sweating and possibly dehydration, which can trigger orthostatic hypotension.
- Alcohol: Drinking alcohol can increase the risk of orthostatic hypotension.
Complications due to Orthostatic Hypotension
Persistent orthostatic hypotension can lead to serious complications, especially in older adults. These include:
- Falls: Falling as a result of fainting is a common complication in people with orthostatic hypotension.
- Stroke: The fluctuations in blood pressure due to orthostatic hypotension can be a risk factor for stroke due to reduced blood supply to the brain.
- Cardiovascular diseases: Orthostatic hypotension can increase the risk of cardiovascular diseases and complications, such as chest pain, heart failure, or heart rhythm problems.
Diagnosing Orthostatic Hypotension
A healthcare provider’s goal in evaluating orthostatic hypotension is to identify the cause and determine the appropriate treatment. The diagnostic process often involves reviewing the patient’s medical history, symptoms, medications, and conducting a physical examination.
Several tests may be recommended to diagnose orthostatic hypotension, such as:
- Blood pressure monitoring: This involves measuring blood pressure while sitting and standing.
- Blood tests: These can provide information about the patient’s overall health, including low blood sugar (hypoglycemia) or low red blood cell levels (anemia).
- Electrocardiogram (ECG or EKG): This test measures the electrical activity of the heart.
- Echocardiogram: This test uses sound waves to create images of the heart in motion.
- Stress test: This test measures how the heart responds to exertion.
- Tilt table test: This test shows how the body reacts to changes in position.
- Valsalva maneuver: This noninvasive test determines how well the autonomic nervous system is functioning.
Treatment for Orthostatic Hypotension
Treatment for orthostatic hypotension is typically directed at the underlying cause. For instance, if dehydration is causing orthostatic hypotension, the healthcare provider may suggest lifestyle changes such as drinking more water. If a medication is causing low blood pressure, treatment may involve adjusting the dosage or discontinuing the medication.
In addition to treating the underlying cause, there are several nonpharmacologic and pharmacologic treatments available to manage the symptoms of orthostatic hypotension. These treatments aim to improve blood pressure, relieve symptoms, and enhance the quality of life for individuals with this condition.
Lifestyle Changes
Certain lifestyle changes can help manage or prevent orthostatic hypotension. These include:
- Wearing waist-high compression stockings: These can improve blood flow and reduce the symptoms of orthostatic hypotension.
- Getting plenty of fluids: Staying hydrated can help prevent symptoms of low blood pressure.
- Avoiding alcohol: Alcohol can worsen orthostatic hypotension, so it’s important to limit or avoid it completely.
- Increasing salt in the diet: This must be done carefully and only after discussing it with a healthcare provider. Too much salt can increase blood pressure beyond a healthy level, creating new health risks.
- Eating small meals: If blood pressure drops after eating, having small, low-carbohydrate meals might help.
- Exercising: Regular cardiovascular and strengthening exercises might help reduce symptoms of orthostatic hypotension.
- Moving and stretching in certain ways: Stretching and flexing calf muscles before standing up can help manage symptoms.
- Getting up slowly: It’s important to move slowly from a lying to standing position to prevent a sudden drop in blood pressure.
- Raising the head of the bed: This can help fight the effects of gravity and reduce the risk of orthostatic hypotension.
Medication
In some cases, medication may be necessary to manage orthostatic hypotension. Potential medications include midodrine, fludrocortisone, droxidopa, and pyridostigmine. It’s important to discuss the risks and benefits of these drugs with a healthcare provider to determine the best treatment option.
Prognosis
Orthostatic hypotension may lead to accidental falls and is also linked to an increased risk of cardiovascular disease, heart failure, and stroke. Furthermore, observational data suggest that orthostatic hypotension in middle age increases the risk of eventual dementia and reduced cognitive function.
Summary:
The article discusses orthostatic hypotension, a condition marked by a sudden drop in blood pressure upon standing. Its causes, symptoms, risk factors, complications, diagnosis, and treatment are explored. Common symptoms include lightheadedness, dizziness, blurry vision, and fainting. Causes range from dehydration to heart problems, and risk factors include age, certain medications, and heat exposure. Complications may involve falls, stroke, and cardiovascular diseases. Diagnosis involves tests like blood pressure monitoring and blood tests. Treatment focuses on managing underlying causes, with lifestyle changes and medications like midodrine and fludrocortisone being potential options. Lastly, the article emphasizes the importance of seeking medical attention for frequent or severe symptoms.
FAQ’S
What are the common symptoms of orthostatic hypotension?
- The common symptoms of orthostatic hypotension include lightheadedness, dizziness, blurry vision, weakness, fainting, and confusion.
How is orthostatic hypotension diagnosed?
- Orthostatic hypotension is diagnosed through blood pressure monitoring, blood tests, electrocardiogram, echocardiogram, stress test, tilt table test, and Valsalva maneuver.
What lifestyle changes can help manage orthostatic hypotension?
- Lifestyle changes such as wearing compression stockings, staying hydrated, avoiding alcohol, increasing salt intake, eating small meals, regular exercise, and moving slowly can help manage orthostatic hypotension.
What are the treatment options for orthostatic hypotension?
- Treatment involves addressing the underlying cause, lifestyle changes, and in some cases, medication such as midodrine, fludrocortisone, droxidopa, and pyridostigmine. All medical treatments should be discussed with a healthcare provider.


